The Ministry of Health & Family Welfare (MoHFW) has detailed protocol & guidelines for the identification, treatment & discharge of COVID-19 suspects & patients. Here is a detailed explainer of the process.
With more than 2500 confirmed COVID-19 cases, India is witnessing a stark increase in the number of cases being. As the outbreak intensifies, the government is making necessary modifications to the procedures to be followed by people, hospitals, and laboratories. In this story, we briefly look at who are tested, and what actions are taken based on result, that is, treatment, and isolation.
Who are tested for COVID-19?
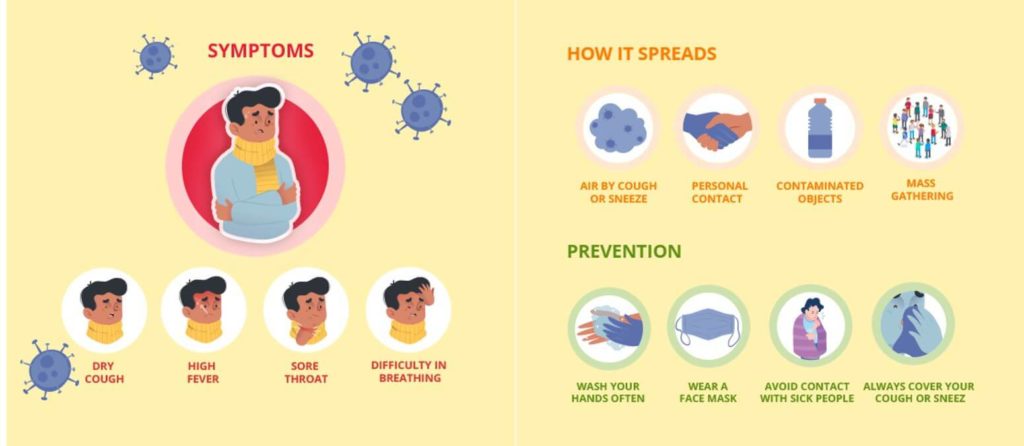
As per the government’s notification on 31 March 2020, the basket of people who are tested for COVID-19 are as follows. Symptomatic individuals are those who have fever, shortness of breath or cough. All the suspected cases must be reported to both district and state surveillance offices.
- All symptomatic individuals who have travelled to or from foreign countries in the last two weeks. (Initially, only those who had travelled to highly affected regions such as China, Italy and Qatar had to get themselves tested.)
- All symptomatic contacts of those persons who have been tested positive for the coronavirus.
- Healthcare personnel who have examined a person with COVID-19, and shows symptoms of the disease
- Asymptomatic persons who belong to the high-risk category or have had direct contact with those tested positive should be tested between 5 to 14 days since the contact was made. This includes persons living in the same house as the confirmed case.

How can one get themselves tested?
Any person with symptoms or has had contact or travel history must approach the nearest health facility. They also have an option to call the helpline numbers released by the government where the call centres enquire demographic details, clinical conditions, symptoms, and whether they were under home quarantine as per local health administration’s directions.
What is the procedure for testing?
Samples are collected from those suspected cases as mentioned above. As per the guidelines issued by the ministry, nasal and throat swabs are the preferred samples to be collected. Nasopharyngeal swab, Bronchoalveolar lavage or endotracheal aspirate are alternative samples that may be collected. The samples collected should be mixed in a viral transport medium and transported on ice to the designated laboratories for testing.
It is mandatory that biosafety and biosecurity precautions are taken at the time of sample collection, packaging and transport. This include usage of appropriate Personal Protection Equipment (PPE) by healthcare professionals who collect the sample from the suspected patient. Visitors should also be restricted at this time. Even waste disposal must be done with utmost care in strict compliance with Biomedical Waste Management Rules, 2016 as the virus is highly contagious.

For each sample being submitted, a requisition form must be filled with details such as personal details of the person whose sample has been taken, date and time of collection, exposure history of the person- clinical symptoms, underlying medical conditions, etc. Also, at the time of sample collection, a government ID proof of residence and contact details of the suspected patient must also be collected. ICMR recommends private laboratories to collect samples from the homes of the persons so as to minimize human contact while traveling and in collection centres. Approval of private labs and details of sample collection and testing have already been covered in an earlier story by Factly.
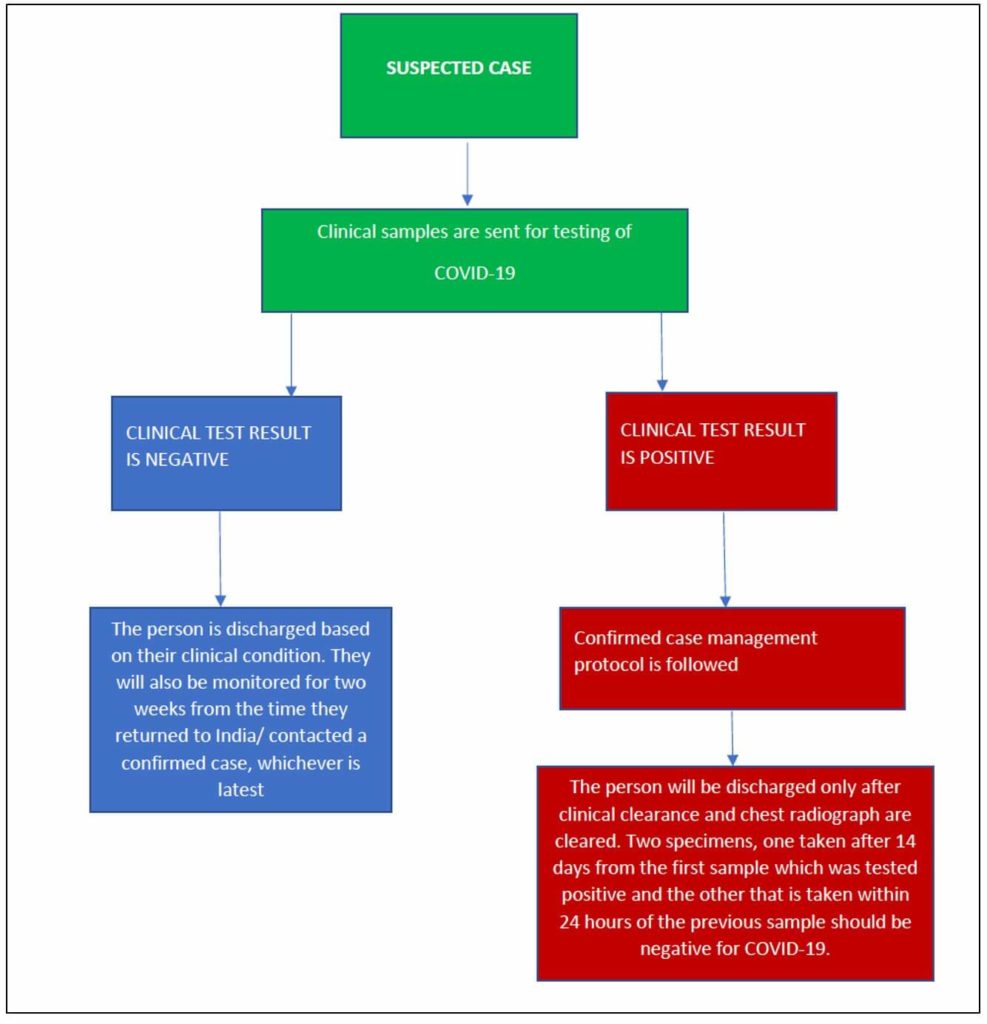
What happens until & after the test result?
Till the laboratory results are out, the person is kept in isolation at the health facility. Treatment will continue for the symptoms they possess.
If the result is negative, the patient is discharged depending on the diagnosis. The doctor can take the call on the required treatment based on the patient’s condition. However, there will be continuous monitoring for fourteen days from the day they returned to India or from the day they made contact whichever is the latest. This is because the incubation period for the virus to affect a person varies between one to fourteen days, though studies suggest that symptoms are seen within 5 days for most people.

How are isolation and quarantine different?
Quarantine is the term used for separation of individuals who have been exposed to an infected person and have a potential to get infected. There will be temporary home quarantine for those who just returned from other countries.
Isolation is the term used for separation of those persons who are ill and are suspected or confirmed cases of COVID-19. So, those suspected cases whose results are awaited and confirmed cases are kept in isolation in hospitals or healthcare centres until they get tested negative for the virus.
What happens if the test result is positive?
For those tested positive, there is a separate confirmed case protocol that is followed. Under this protocol, the drugs to be used for treatment and various measures to contain the virus in hospitals and clinics have been listed. As per the protocol, there are different therapeutic measures given for patients depending on the severity of the illness-mild, moderate, and severe. Co-morbid condition of the patient is also considered for the treatment. The guidelines recommend pro-active communication with patients and families to provide support and prognostic information. The patient’s values and preferences must also be considered with respect to life-sustaining interventions.
Earlier, the ministry had recommended the use of anti- HIV drugs for the treatment of COVID-19 on a case to case basis. However, this recommendation has been repealed. As per the latest clinical management guidelines, hydroxychloroquine in combination with azithromycin has been recommended for treatment of persons who have severe suffering and those kept under ICU management. Further, Hydroxychloroquine, which is normally used for the treatment of malaria, has been listed as Schedule H1 drug under Drugs and Cosmetics Rules, 1945. In simpler terms, the drug cannot be purchased over the counter without a prescription.
When is the person discharged?
The person will be discharged only after chest radiograph is clear and two respiratory samples within 24 hours are tested negative for SARS-CoV-2 virus. That is, two samples will be collected from the person-
- one after 14 days from the time the first sample was collected which was tested positive
- and the other, within 24 hours from when the previous sample was collected
Both of these samples should show negative results. Only then the person is discharged.